Mechanism of Breathing
Last Updated :
13 Jan, 2024
Mechanism of Breathing is the process by which organisms inhale oxygen and release carbon dioxide. It involves the inhalation of air, where the diaphragm and intercostal muscles expand the chest cavity, allowing air to fill the lungs. During exhalation, the muscles relax, decreasing lung volume and expelling carbon dioxide. The respiratory center in the brainstem regulates this rhythmic cycle. The gaseous exchange takes place in the alveoli, where oxygen diffuses into the bloodstream, and carbon dioxide is released for removal.
Intrapleural breathing helps in maintaining respiratory efficiency. This rhythmic process ensures a continuous exchange of gases necessary for cellular function. In this article, we will discuss breathing, the mechanism of breathing, and Intrapleular breathing in detail.
What is Breathing?
Breathing or respiration, is a process that involves the process of inhalation and exhalation of gases. It takes place in the lungs, where gaseous exchange occurs. Inhalation starts with the contraction of the diaphragm and intercostal muscles, which expands the chest cavity. Due to this, the pressure inside the lung decreases causing air to rush in. Oxygen is then transported to tissues through the bloodstream, while carbon dioxide, a metabolic waste product, is carried back to the lungs. Exhalation involves the relaxation of muscles, reducing lung volume, and expelling carbon dioxide.
Gas exchange in the lungs occurs in millions of small air sacs called alveoli. The breathing rate is the number of breaths taken per minute which is around 12 to 20 breaths per minute. It increases during running, or after exercise and decreases at rest.
Mechanism of Breathing
The mechanism of breathing involves inhalation and exhalationo. The lung volume changes and allow the exchange of gases to support cellular function. The mechanism of breathing takes place in the following steps:
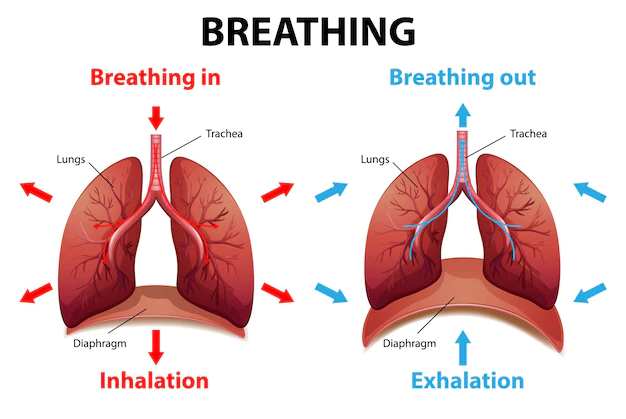
Inhalation
This process involves the intake of air into the lungs. It is initiated by the contraction of the diaphragm, a dome-shaped muscle at the base of the chest, and the external intercostal muscles, which are located between the ribs. As these muscles contract, the chest cavity expands, causing a decrease in air pressure in the lungs. Air then rushes in through the nose or mouth to equalize the pressure, and oxygen is absorbed into the bloodstream.
Also Read: Blood
Mechanism of Inhalation
The mechanism of inhalation is as follows:
- The intake of atmospheric air into the lungs is known as inspiration.
- It is an active process requiring the contraction of specific respiratory muscles.
- During inspiration, the volume of the thoracic cavity increases.
- Contraction of the external intercostal muscles contributes to the expansion of the thoracic cavity.
- The diaphragm, respiratory muscle, contracts during inspiration.
- The combined action of external intercostal muscle contraction and diaphragm contraction increases the size of the thoracic cavity.
- Simultaneously, the lungs expand as the thoracic cavity enlarges.
- The expansion of the lungs results in a decrease in air pressure inside the lungs.
- As a consequence of the decreased lung pressure, atmospheric air rushes inside the lungs to equalize the pressure.
Exhalation
This is the expulsion of air from the lungs. It occurs when the diaphragm and external intercostal muscles relax, allowing the chest cavity to decrease in size. This reduction in volume increases the air pressure within the lungs, causing the air, now rich in carbon dioxide, to be pushed out. Exhalation is a passive process during rest, relying on the elastic recoil of the lungs and chest wall. During physical activity or labored breathing, additional muscles may be involved in the exhalation process.
Mechanism of Expiration
The mechanism of expiration is as follows:
- The process of exhaling carbon dioxide is called expiration. It is a passive process.
- It occurs when the size of the thoracic activity decreases and the air pressure outside increases.
- Now the external intercostal muscles relax and the internal intercostal muscles contract.
- As a result, the ribs are pulled inwards and the size of the thoracic cavity is reduced.
- The diaphragm is relaxed, and the lungs get compressed.
- Consequently, the pressure increases, and the air is forced outside.
Mechanism of Respiration
The mechanism of respiration involves both breathing and gas exchange at the cellular level. The gaseous exchange take place at the surface of alveoli by the process of diffusion. It depends upon the pressure differences between blood and tissues. The mechanism of breathing has already been explained above. We will discuss the steps involved in the exchange of gases.
Exchange of Gases
The exchange of the gases take place in the following steps:
- Oxygen in the blood is carried in two forms: as oxyhemoglobin (oxygen bound to hemoglobin) and dissolved in the blood plasma.
- Oxyhemoglobin forms when the oxygen concentration is high in the blood.
- Oxyhemoglobin dissociates in response to low oxygen levels, low pH, and high temperatures, releasing oxygen.
- Internal respiration in tissues involves the dissociation of oxyhemoglobin, where oxygen is released and used in cellular processes.

Internal Respiration
The gaseous exchange taking place in the tissues is called internal respiration. It takes place inthe following steps:
- In tissues, the dissociation of oxyhemoglobin releases oxygen, which participates in cellular respiration.
- Oxygen breaks down glucose, releasing carbon dioxide, water, and energy.
- The energy is utilized by the body, and carbon dioxide diffuses from the tissues.
Also Read: Diffusion
Transport of Carbon Dioxide from Tissues to Lungs
Carbon dioxide is transported to the lungs, where it is released from the body through expiration. Carbon dioxide is transported in three ways:
- Dissolving in plasma to form carbonic acid.
- Carbonic acid ionizes to form bicarbonate ions with the help of the enzyme carbonic anhydrase.
- Some carbon dioxide combines with hemoglobin to form carbaminohemoglobin.
Intrapleural Breathing
Intrapleural breathing is an important part of the respiratory mechanism, and is used to refer to the pressure that is present in the space between the pleura and the lungs. As the diaphragm and external intercostal muscles contract during inhalation, the thoracic cavity expands, creating a lower pressure in the intrapleural space. This negative intrapleural pressure helps to uphold the adherence between the visceral and parietal pleurae, preventing lung collapse and maintaining optimal lung expansion. The lowered intrapleural pressure help in expanding the lungs, that allow the intake of air for oxygen exchange.
During exhalation, relaxation of respiratory muscles increases intrapleural pressure, helping in elastic recoil and the expulsion of air from the lungs. Intrapleural breathing is essential for maintaining respiratory efficiency.
Respiratory Gas Transport
Oxygen is absorbed, and carbon dioxide is expelled during gas exchange in the lungs. Oxygenated blood is transported from the lungs to the body’s tissues. Deoxygenated blood needs to be returned to the lungs for the cycle to continue. The cardiovascular system, including blood vessels and the heart, plays a crucial role in the transportation of gases. Blood carrying oxygen leaves the lungs and flows into the heart through the pulmonary veins. From the left atrium, oxygenated blood is pumped into the left ventricle of the heart. The left ventricle then ejects oxygenated blood into the aorta and its corresponding branches, facilitating distribution to the rest of the body.
Key Points on Mechanism of Breathing
The key points on mechanism of breathing are:
- During inhalation diaphragm contracts and chest cavity expands. External intercostal muscles causes the ribs to lift and lower the air pressure inside that draws the oxygen inside the lungs.
- During ehalation diaphragm and intercostal muscles relax. Chest cavity reduces in volume, which increases air pressure inside that causes the air to move outside.
- Brainstem regulates breathing rate and depth and responds to blood oxygen and carbon dioxide levels.
- Oxygen is carried by the hemoglobin (oxyhemoglobin) and get dissolved in blood plasma.
- Carbon Dioxide dissolves in plasma, forms bicarbonate and combines with hemoglobin (carbaminohemoglobin).
Also Read:
FAQ’s – Mechanism of Breathing
1. What is Normal Breathing?
Normal breathing involves rhythmic inhalation and exhalation at a rate of approximately 12 to 20 breaths per minute. It maintains a balance of oxygen and carbon dioxide in the bloodstream to support various body functions. The process is controlled by the respiratory center in the brainstem.
2. What are the 4 Steps of Breathing?
The process of breathing occur thorugh inhalation and exhalation. These processes occur in four steps: Ventilation, Pulmonary gas exchange, Gas transport, Peripheral gas exchange.
3. What is the Mechanism of Breathing?
The mechanism of breathing involves inhalation, where the diaphragm contracts, expanding the chest cavity, and exhalation, as muscles relax, reducing lung volume and expelling air containing carbon dioxide. This rhythmic process ensures continuous gas exchange for cellular respiration.
4. What are the Function of the Lungs?
The main function of the lungs is to delivers oxygen to the cells in your body. Removes waste gases, including carbon dioxide, from the body when you exhale. Protects your airways from harmful substances and irritants
5. What is Alveoli?
Alveoli are tiny air sacs in the lungs where gaseous exchange take place. Oxygen enters the bloodstream and carbon dioxide is released. It provide a large surface area for efficient exchange of gases.
Like Article
Suggest improvement
Share your thoughts in the comments
Please Login to comment...